
Suspected allergic contact dermatitis after skin closure with 2-octylcyanoacrylate: a case report
Highlight box
Key findings
• Gynecologic surgery patients may be sensitized to octyl cyanoacrylate tissue adhesive (skin glue) from prior exposures subsequently predisposing them to allergic contact dermatitis (ACD) that may impede surgical healing.
What is known and what is new?
• As skin glue becomes more popular due to decreased cost and operative time, the risk of sensitization also increases, particularly for those with repeat exposure to cyanoacrylates.
What is the implication, and what should change now?
• This case highlights the need for gynecologic surgery providers to perform detailed preoperative evaluation of prior allergic symptoms and exposure history. Providers should also counsel the patient on signs and symptoms of ACD to increase postoperative surveillance and be aware of ACD treatment regimens. Providers may consider using alternatives to skin glue.
Introduction
Cyanoacrylates are chemical compounds that are commonly used in glue and polymerize upon contact with moisture to form a cohesive sheet (1). 2-octylcyanoacrylate was first approved by the Food and Drug Administration in 1998 for use as a topical skin adhesive for surgical incisions, including minimally invasive puncture sites and lacerations with clean edges (1). The applied layer of 2-octyl cyanoacrylate peels off over 2 weeks as the epidermal layers regenerate (1). Allergic contact dermatitis (ACD) after exposure of skin adhesives is a potential adverse event. While cyanoacrylate is the predominant ingredient of commercial skin adhesives with concentrations ranging from 78% to 99%, it is important to consider all components of skin adhesive for allergen potential (2). In addition to cyanoacrylate, skin adhesives may also contain the following compounds: formaldehyde impurities, hydroquinone, butylated hydroxyanisole (BHA), butylated hydroxytoluene (BHT), sulfur dioxide, polymethacrylates, polycyanoacrylates, polyacrylates, tributyl citrate, tributyl acetyl citrate, and synthetic violet dye (2). Studies have shown that patients are allergic to the cyanoacrylate component of skin adhesives and thus, allergic potential to cyanoacrylates must be carefully considered when choosing skin closure methods (1,2).
Exposure to skin glue or compounds present in skin glue may lead to the development of ACD in patients. The incidence of ACD after exposure to skin adhesives in the gynecological surgery population is largely unknown, but studies suggest sensitization to skin glue occurs at a higher ratio of females to males (3,4). Given the widespread use of skin glue, gynecological surgery patients may be at an increased risk of developing ACD. This case demonstrates the suspected development of ACD after exposure to skin glue that persisted for months and required medical management. Surgical providers may avoid this risk by considering the use of traditional suture closures in patients with risk factors for developing ACD. Providers should be aware of this potential risk and counsel patients appropriately regarding their prior experiences with skin glue and other adhesives. We present this article in accordance with the CARE reporting checklist (available at https://gpm.amegroups.org/article/view/10.21037/gpm-23-20/rc).
Case presentation
This patient was a 46-year-old female who presented with stage II posterior-predominant uterovaginal prolapse and stress urinary incontinence. Her past surgical history is notable for laparoscopic ventral hernia repair in 2019 and a revision of mesh disruption in 2020. The patient reports that she experienced itching around the abdominal incisions after the hernia repair and mesh revision. She states that she used ice packs to manage her pruritis at the time and that she did not report her symptoms to a provider. Notably, the patient often wore artificial nails with acrylate containing glue many years ago with no allergic reaction. She reports that she has never had any reactions to hot glue (used in glue guns), latex, vinyl, paint, or gel nail polish. She reports history of allergy to grass and dust. The patient and her surgeon elected to proceed with laparoscopic supracervical hysterectomy, bilateral salpingectomy, sacrocolpopexy, posterior colporrhaphy, perineorrhaphy, retropubic midurethral mesh sling, cystourethroscopy for management of her pelvic organ prolapse and stress urinary incontinence.
Immediately prior to start of surgery, chlorhexidine was used for the abdominal prep. The patient was given intravenous cefotetan for surgical antibiotic prophylaxis intraoperatively, and the surgery itself was uncomplicated. Five laparoscopic incisions and two suprapubic incisions were closed with subcuticular stitches of polysorbate suture and 2-octylcyanoacrylate skin glue. Patient was discharged to home on postoperative day #0.
The patient called into the nurse triage line on postoperative day #6 to report that two of her seven laparoscopic sites (the left lateral port and supraumbilical incision) were itchy and draining. The nurse recommended cool packs and over-the-counter diphenhydramine if pruritis became severe. That same day the patient sent in some photographs through the hospital portal system (Figure 1). After review by one of the clinical fellows, it was recommended she try over-the-counter hydrocortisone cream as needed and schedule an appointment to be seen. Later that day the surgeon called the patient as a video-call and the patient confirmed her erythematous incisions. ACD to skin glue was suspected as the most likely diagnosis at this time by the surgeon who advised the patient to apply topical hydrocortisone twice daily to the incision sites. On postoperative day #8, the patient sent follow-up photographs to demonstrate her progress after treatment with oral diphenhydramine and topical hydrocortisone (Figure 2).

On postoperative day #9 at her office visit, the patient reported persistent itching at all her laparoscopic port sites despite the use of hydrocortisone and diphenhydramine. On physical examination, the patient had an intact subumbilical incision covered in skin glue with blanching erythema extending 4 to 5 cm circumferentially around the incision, an intact supraumbilical incision with blanching erythema extending 3 to 4 cm circumferentially, and five other intact laparoscopic sites with blanching erythema extending 1 to 2 cm circumferentially around the incisions. There was also mild induration of the subumbilical incision without fluctuance. There was mild erythema that was lacy in appearance around the retropubic trocar incision sites. The patient had normal vital signs and denied intraabdominal pain, so suspicion for intraabdominal infection was low. The physician attempted glue removal after application of bacitracin ointment to facilitate removal due to suspicion of glue allergy, but this was unsuccessful. The physician proceeded to treat the patient for presumed ACD with a methylprednisolone dose pack to address symptoms of persistent pruritis and allergic reaction. Sulfamethoxazole-trimethoprim 160–800 mg twice daily for 7 days was also prescribed due to concern for underlying superficial cellulitis.
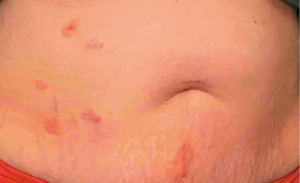
On postoperative day #13 during a telephone encounter, the patient reported improvement in pruritis, but emergence of a new maculopapular rash around the incision sites. On postoperative day #14 via telephone encounter, the patient reported that the maculopapular rash extended to the upper inner thighs. She stopped taking trimethoprim-sulfamethoxazole on day #14 due to the concern for a drug reaction with new rash. The surgeon advised the patient to apply petroleum jelly to facilitate removal of the remaining skin glue and prescribed triamcinolone ointment to apply twice daily over pruritic incision sites.
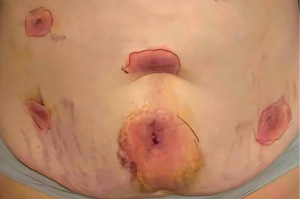
Postoperative day #21, the patient reported worsening skin irritation of the abdomen despite triamcinolone use. Diphenhydramine was increased from 25 to 50 mg once daily. On postoperative day #26, patient reported worsening of the maculopapular rash (Figure 3). At her scheduled 6-week postoperative office visit, she was noted to have mild erythema around her incisions and the supraumbilical incision had a small excoriation on physical examination.
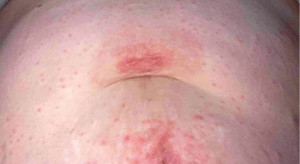
Six months postoperatively, the patient noted recurrence of urticarial rash adjacent to the incision sites and umbilical pruritis (Figure 4). She received prednisone at an urgent care facility, and continued diphenhydramine. Shortly after, she visited an allergist who noted ongoing incisional ACD and recommended treatment with high dose, nonsedating oral antihistamines and a topical triamcinolone cream. While she has not taken this, she has taken cetirizine daily and notes that she gets hives if she stops taking it. Two resolving areas of urticaria adjacent to incision sites were seen at the 7-month postoperative visit by the operating surgeon. She had been recommended to follow-up with dermatology for contact dermatitis patch testing by her surgeon but reports that the dermatologist had not recommended any patch testing.
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Discussion
Gynecological surgery patients may be sensitized to octyl cyanoacrylate tissue adhesive (skin glue) from prior exposures subsequently predisposing one to ACD that impedes surgical healing. This patient had a history of acrylic nail use as well as a prior sensitization to skin glue which may have resulted in ACD.
The degree to which this patient was exposed to 2-octylcyanoacrylate with her acrylic nail use or from prior skin glue use is not known. However, it is likely that many patients are not aware of their exposure to this substance, so this case may be representative of the general population. Additionally, since the patient did not proceed with patch testing, the exact compound in the skin glue that caused the reaction cannot be confirmed.
Multiple cases of ACD after using skin adhesive use have been noted in the literature, however the incidence remains unclear. In a 2021 study by Park et al. of patients who underwent orthopedic surgery, 29 of 1,145 of patients (2.5%) were diagnosed with ACD after use of cyanoacrylates (5). In a study of 100 women by Nakagawa et al. who underwent breast surgery, 7% had contact dermatitis after exposure to 2-octylcyanoacrylate (4). Another study by Fluellen et al. specifically looking at patients with exposure to 2-octylcyanoacrylate during urogynecologic surgery reported 0% incidence of ACD in 23 patients (6). However, this study is limited due to its small sample size with a cohort of 23 participants (6). A significant risk factor for ACD from cyanoacrylates is prior exposure, as seen in this case. In a study performed by Muttardi et al., sensitization to acrylates was seen with a ratio of 15:1, females to males, with known past exposures to nail glue, eyelash glue, acrylic/gel nails, and surgical drapes (3). In patients who were sensitive to 2-octylcyanoacrylate, 37% were also allergic to acrylates, which are commonly used in cosmetics (2). While Park et al. found no association with sex, the higher incidence seen in Nakagawa et al.’s study and the ratio of sensitization seen in Muttardi et al.’s study suggest sex as a risk factor (3-5). Larger scale retrospective studies are required to understand the true incidence and sex specific risk factors of ACD after exposure to 2-octylcyanoacrylate.
Use of cyanoacrylate skin glues for skin closure is advantageous as it has been shown to decrease closure time and cost. Studies have shown laparoscopic trocar site closure time is 10 to 20 minutes less with skin adhesive, and that the average cost of skin adhesive for closure was also less than half of the cost compared to suture material (6,7). Additionally, an in vitro study has shown that skin adhesive has bactericidal properties against gram positive bacteria and an animal study has shown decreased growth of microorganisms postoperatively (8,9). As skin adhesive becomes more popular given these positive attributes, the risk of sensitization also increases, indicating the possibility of an increasing incidence of ACD in coming years, particularly for those with repeat exposure to cyanoacrylates. One study showed that 57% of patients with ACD after skin glue use had prior exposure to 2-octylcyanoacrylate (4). Patients may not share prior dermatological concerns if not prompted, or they may not be aware of risk factors for ACD development and prior exposures.
This case highlights many considerations for gynecologic surgeons including preoperative evaluation, postoperative surveillance, and treatment regimens for ACD. Preoperative evaluations should include detailed history of allergies, note of prior cyanoacrylate exposure, as well as use of similar glues in cosmetics and crafts. It is also important to counsel the patient on signs and symptoms of ACD so that early detection and early interventions can be executed. Explicitly asking about incisional pruritis may elicit disclosure of symptoms which may have otherwise been ignored by patients as something that is insignificant. In this case, knowledge of the prior 2-octylcyanoacrylate sensitization and reaction would have excluded skin adhesive use and led to better surgical outcomes. The treatment for this patient required use of topical and systemic steroids. While human studies have shown acute corticosteroid use of less than 10 days to have no clinically significant effect on wound healing, direct effect on mesh complications is unknown (10). Given this, the authors recommend maintaining a heightened awareness of the potential for ACD with skin glue use as well as the use of topical steroids over systemic steroid when possible.
Conclusions
Given the ease of use, decreased operative time, and decreased cost of tissue adhesive when compared to sutures, tissue adhesive may be a favorable form of closure for many surgeons. However, this also means more surgical patients may have prior exposure to skin adhesives, higher likelihood of sensitization, and greater risk for ACD. Providers should consider an individual’s risk for ACD when choosing skin closure methods. Overall, careful consideration for ACD preoperatively and evaluation postoperatively are of great importance for better operative outcomes.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at https://gpm.amegroups.com/article/view/10.21037/gpm-23-20/rc
Peer Review File: Available at https://gpm.amegroups.com/article/view/10.21037/gpm-23-20/prf
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://gpm.amegroups.com/article/view/10.21037/gpm-23-20/coif). M.F.A. is supported by NIH National Institute on Aging (Nos. R03AG064378-01, K23AG073517-01), Alzheimer’s Association, and the Pennsylvania Department of Health (No. 4100088553). M.F.A. declares that these grants/funds are not used to prepare the manuscript. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Singer AJ, Thode HC Jr. A review of the literature on octylcyanoacrylate tissue adhesive. Am J Surg 2004;187:238-48. [Crossref] [PubMed]
- Cook KA, White AA, Shaw DW. Patch Testing Ingredients of Dermabond and Other Cyanoacrylate-Containing Adhesives. Dermatitis 2019;30:314-22. [Crossref] [PubMed]
- Muttardi K, White IR, Banerjee P. The burden of allergic contact dermatitis caused by acrylates. Contact Dermatitis 2016;75:180-4. [Crossref] [PubMed]
- Nakagawa S, Uda H, Sarukawa S, et al. Contact Dermatitis Caused by Dermabond Advanced Use. Plast Reconstr Surg Glob Open 2018;6:e1841. [Crossref] [PubMed]
- Park YH, Choi JS, Choi JW, et al. Incidence and risk factor of allergic contact dermatitis to 2-octyl cyanoacrylate and n-butyl cyanoacrylate topical skin adhesives. Sci Rep 2021;11:23762. [Crossref] [PubMed]
- Fluellen S, Mackey K, Hagglund K, et al. Randomized clinical trial comparing skin closure with tissue adhesives vs subcuticular suture after robotic urogynecologic procedures. World J Methodol 2020;10:1-6. [Crossref] [PubMed]
- Sebesta MJ, Bishoff JT. Octylcyanoacrylate skin closure in laparoscopy. J Endourol 2003;17:899-903. [Crossref] [PubMed]
- Rushbrook JL, White G, Kidger L, et al. The antibacterial effect of 2-octyl cyanoacrylate (Dermabond®) skin adhesive. J Infect Prev 2014;15:236-9. [Crossref] [PubMed]
- Basaran M, Kafali E, Ugurlucan M, et al. Cyanoacrylate gluing increases the effectiveness of systemic antimicrobial treatment in sternal infection: experimental study in a rodent model. Thorac Cardiovasc Surg 2008;56:28-31. [Crossref] [PubMed]
- Wang AS, Armstrong EJ, Armstrong AW. Corticosteroids and wound healing: clinical considerations in the perioperative period. Am J Surg 2013;206:410-7. [Crossref] [PubMed]
Cite this article as: Patnaik S, Melnyk AI, Vargas LG, Ackenbom MF. Suspected allergic contact dermatitis after skin closure with 2-octylcyanoacrylate: a case report. Gynecol Pelvic Med 2023;6:31.


